The term “adrenal dysfunction” can include conditions like Addison’s disease (not enough cortisol) and Cushing’s disease or syndrome (too much cortisol). But those are fairly rare, advanced stages of adrenal pathology that are largely rooted in immune system dysfunction (these conditions are usually caused by autoimmunity and tumors).
And while ANY condition can be impacted by stress, this article is focused on functional adrenal issues that develop over time from a “maladaptive stress response.” Maladaptive, meaning your mental-emotional-physical response to the stress was dysfunctional. This is usually because the way you responded to that stress was in direct conflict with what your body needs to be healthy.
Now I don’t say that to shame or blame you! Some simple examples of stress responses that undermine health—that we’ve ALL done at some point—include: skimping on sleep, rushing through meals, sitting too much, staying up late, choosing foods that are high in calories and low in nutrients (like sugary treats and refined carbs), drinking too much coffee, or turning to alcohol.
But when we respond to stress in a way that creates dysfunction in these foundational areas of health (sleep, food and blood sugar/insulin, activity level, etc.), AND when that dysfunction becomes a pattern, it will eventually impact how our brain and adrenals communicate—which leads to chronic dysfunction in how the adrenal glands behave.
To put it another way, when we let stress mess with the areas of our health that are absolutely necessary and foundational for our wellbeing, this can cause chronic issues over time that include adrenal dysfunction.
Since cortisol is the major adrenal hormone involved in our stress response, these changes in brain-adrenal communication can affect how much cortisol the adrenals secrete, and when. So what should the adrenals be doing when it comes to cortisol?
Normal Cortisol Rhythm
A healthy and normal cortisol rhythm looks like this:
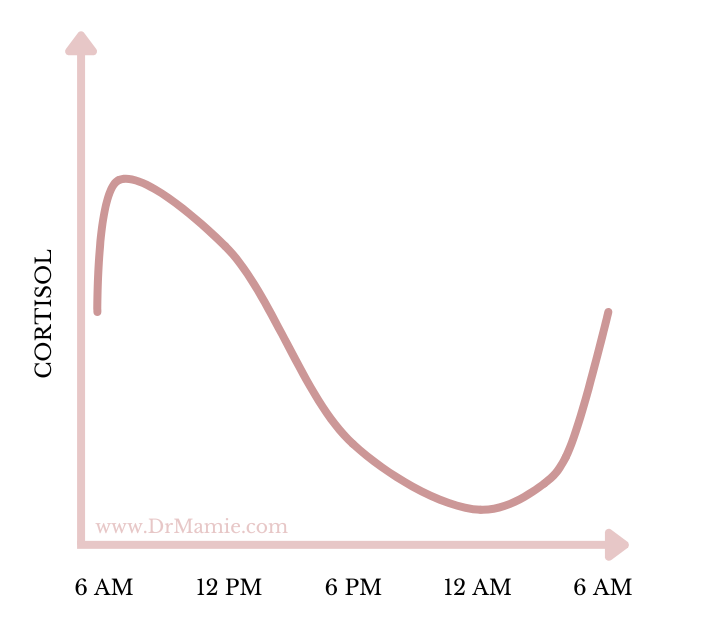
Your cortisol levels are highest in the morning soon after waking and gradually taper off during the day so they are lowest at night, especially during the first few hours of sleep. In the wee hours of the morning, cortisol levels rise, and at a certain threshold the cortisol helps you wake up—refreshed.
But adrenal dysfunction can create levels of cortisol that are too low, too high, or a mixture of abnormal levels. So let’s look more closely at how out-of-whack cortisol can affect your health.
What Does Adrenal Dysfunction Look Like?
There are several clues that can point to non-optimal or abnormal cortisol levels. Keep in mind that many of these symptoms can be caused or worsened by other imbalances, so it’s best to work with a provider who understands your whole health picture.
Clues You Have Low Cortisol
- Difficulty staying asleep
- Cravings for salt or salty foods
- Slow starter in the morning, hard to get going
- Afternoon fatigue
- Dizziness when standing up quickly
- Afternoon headaches
- Headaches with exertion or stress
- Weak nails
How Low Cortisol Affects Other Areas
- Lower cortisol from adrenal hypofunction leads to low blood sugar. Low blood sugar is a stressor that then triggers the adrenals to release cortisol, leading to insulin resistance over time.
- Low cortisol makes it harder to regenerate the lining of your intestines. Over time, this can lead to leaky gut, ulcers, and new or worse food intolerances.
- Inadequate cortisol can impair liver detox.
Clues You Have High Cortisol
- Difficulty falling asleep
- Sweating easily or from little or no activity
- Excessive sweating
- Under a high amount of stress
- Gain weight when under stress
- Wake up tired even after 7-8 hours of sleep
How High Cortisol Affects Other Areas
- Adrenal hyperfunction leads to excess cortisol and insulin resistance. Insulin then activates a pathway that further promotes adrenal hyperfunction in a vicious cycle.
- High cortisol causes increased breakdown of the intestinal lining, which can lead to leaky gut, ulcers, and new or worse food intolerances.
- The insulin resistance caused by adrenal hyperfunction can impair liver detox.
- High cortisol can promote thyroid dysfunction, specifically “secondary hypothyroidism” and issues converting T4 into T3 (learn about the 6 different types of hypothyroidism here).
- Too much cortisol decreases the amount of FSH and LH that your brain secretes, which then lowers estrogen and progesterone levels. High levels of cortisol can even disrupt the process of ovulation and therefore affect your periods and fertility (and if you don’t ovulate, you don’t make any progesterone—which means you miss out on all the benefits of this important sex hormone!).
- Excess cortisol suppresses the immune system and can lead to low white blood cells (WBCs).
- Even though cortisol is a natural anti-inflammatory, too much of it actually increases inflammation and the production of inflammatory cytokines.
- High levels of cortisol increase the risk of autoimmunity.
- Chronically elevated cortisol can contribute to osteopenia or osteoporosis. This is because high cortisol can cause calcium malabsorption, activate osteoclasts (which break down bones), and decrease bone mineral density.
- Cortisol levels that are too high damage the hippocampus and cause it to atrophy (shrink and waste away). The hippocampus is a part of your brain involved in your circadian rhythm and memory. It’s important to note that the first target of Alzheimer’s disease is the hippocampus!
Adrenal Dysfunction Can Be A Mix of Highs + Lows
The reality is you may be dealing with cortisol levels that are too low, too high, a mix of high and low, or a mix of normal levels with highs and/or lows.
Just about any pattern you can imagine is possible, but when I was regularly testing patients, I most commonly saw a flipped cortisol pattern: too low in the morning and too high at night. Speaking of testing…
Adrenal Testing
When assessing functional adrenal imbalances, there are three options for testing: serum (blood draw), 4-point saliva, and 4-point urine (“4-point” meaning four separate samples are taken throughout the day).
Each testing method provides different insight:
- Serum testing tells you about your total cortisol production at the time of your blood draw.
- Salivary testing tells you how much cortisol is free (meaning the amount of cortisol that is not bound to protein, so it’s “free” and able to interact with receptors). Because four different samples are collected, you get an idea of your free cortisol levels throughout the day.
- Urinary testing tells you about your free cortisol, cortisone (inactive cortisol), and how your body is metabolizing cortisol. Four samples are collected to map your levels over the course of a day.
This means to really know what’s going on, you would ideally get both serum (blood) and 4-point urinary cortisol testing.
But as you can imagine, these tests can add up quickly—especially when there are other areas of your health that need to be evaluated, too!
Which is why I have a very thorough intake process! Taking a good history, analyzing food and lifestyle habits, discussing stressors and stress management—this is all very insightful, and your doctor should be talking about that with you!
Then I top it off by analyzing bloodwork from a functional perspective, which helps to reveal imbalances that are simmering below the surface and can even point to adrenal dysfunction!
With this comprehensive approach, I often get the info I need without doing any adrenal testing.
You’ve Got Adrenal Dysfunction—Now What?
At this point, you’ve probably realized you have some adrenal dysfunction going on! Welcome to the club! 😅 Now the big question is what can you do about it?
It turns out—a LOT! Check out my article How to Heal Adrenal Dysfunction to learn more.
AND, if you haven’t snagged my guide 4 Steps to Skyrocket Your Energy, then you better get on that because I teach you some of the most effective ways to support your blood sugar regulation and adrenal function (which are intimately connected, as you learned in “Adrenal Fatigue” + Why It Happens).
Want personalized guidance? Learn how my approach can help you optimize adrenal function and overall health here.

+ show Comments
- Hide Comments
add a comment